Having an Oesophageal Dilatation
Please note, this page is printable by selecting the normal print options on your computer.
Introduction
You may have been having problems with your swallowing and your hospital doctor has suggested that having an oesophageal dilatation will help improve these difficulties. This procedure requires your formal consent. This booklet has been written to enable you to make an informed decision in relation to agreeing to the investigation and treatment. You will be required to sign a consent form on the day of the procedure, which is a legal document, therefore please read this booklet carefully. If you are unable to keep your appointment, please notify the endoscopy unit as
soon as possible. This will enable staff to give your appointment to someone else and to re-arrange another date and time for you.
You need to understand all the information, including the possibility of complications. There will be the opportunity to speak to a health care professional about anything that you do not understand on the day of the procedure before you sign the consent form.
What is an Oesophageal dilatation?
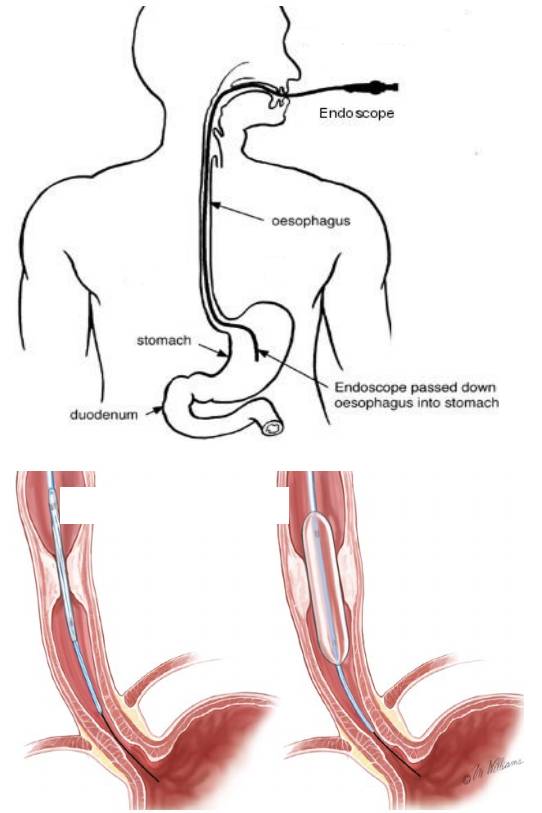
The oesophagus, or gullet, is the tube that takes food down from the mouth to the stomach. If it becomes narrowed or blocked, there will be a problem with swallowing. Oesophageal dilatation is a procedure that widens a narrowing in your oesophagus using a special catheter (long, thin tube) with a balloon attached. Dilatation should stretch the narrowing and make it easier for you to swallow. More than one dilatation may be needed over several appointments depending on how much stretching your oesophagus is required.
Are there any alternatives to having an Oesophageal dilatation?
The aim of the dilatation is to allow you to swallow more easily again. There is no alternative procedure that can be done to stretch the oesophagus to allow you to swallow better. If you decided against having this procedure and you can no longer swallow the nutrition the normal way; there are alternatives available, but these are not appropriate for everybody. You’ll need to discuss these with your consultant.
What will happen when I arrive?
You will be admitted to hospital on the day before your procedure. (Very occasionally, it may be the morning of your procedure). This is so that you can be seen by a doctor and have blood tests (if required) taken before you have the procedure. You will be advised to fast for six hours before the procedure. This means no food or drink. This is so that your stomach is empty. Before you have the procedure, the doctor will ask you to sign a Consent Form. He will explain the procedure again and answer any questions you may have. He will also explain any potential risks.
The Doctor or nurse will also put a small needle in a small vein either on the back of your hand or in your arm. This will enable you to have some medication (sedation) which will help you relax during the procedure. You will not be asleep.
The procedure
When it is your turn you will be taken to the Endoscopy procedure room; you will be introduced to the team and a verbal safety checklist (called “WHO”) will be done. Your throat will be made numb by using the local anaesthetic spray; you will then be asked to lie on your left side. A “probe” will be placed on your finger which can read your pulse and the amount of oxygen in your body (pulse oximeter). Oxygen will be given, usually via a sponge which is placed into one of your nostrils. A mouth guard is placed lightly between your teeth. The Doctor passes a flexible tube (endoscope) down through your throat, into your gullet and assess the narrow area. A balloon catheter is then passed down the narrow area. When the balloon is in the correct position, it is expanded to stretch the narrowing. This may be repeated a number of times. Once the doctor is happy with the dilatation; the endoscope is then gently passed across the dilated area to examine the stomach and duodenum. The procedure should take about 20 minutes.
Will it hurt?
Sometimes people experience chest or back pain. This can vary and may be only discomfort. This usually settles within a couple of hours to a day. Please let your nurse and/or doctor know if you do have discomfort or pain as pain relief medication can be given to help you feel more comfortable.
Aftercare
After your procedure you may have a chest x-ray to check. This is important. Your nurse will tell you when you are allowed to have a drink and something soft to eat. This may be a few hours. Before you go home the Dietitian and/or your key worker (your Upper GastroIntestinal (UGI) Nurse Specialist) may come and talk to you about types of food you can have and give you some simple tips on how to keep your stent clean. This is mainly about having plenty of fluids to drink, particularly with your meals. Please be aware that there will be some types of food that you will still need to avoid.
Here are some simple tips:
• Sit upright to eat
• take small mouthfuls of food
• eat slowly and chew your food well
• use plenty of sauces, gravy and butter to moisten food
• if your appetite is poor, consider having smaller and more frequent nourishing meals
Are there any risks?
Having an Oesophageal dilatation does have some risks associated with it. These occur infrequently, but we wish to draw your attention to them in order to help you make your decision. The doctor or specialist nurse who has requested the test will have considered this already. The risks must be compared with to the benefit of having the procedure carried out. The risks can be associated with the procedure itself and the administration of the sedation.
Complications can happen. The possible complications are listed below. Any numbers which relate to risk are from studies of this procedure. Your doctor will tell you if the risk of complications is higher or lower for you.
• Sore throat, which gets better quickly
• Allergic reaction to equipment, materials or sedative. The endoscopy team is trained to detect and treat any reaction that may happen. Let the admitting nurse and endoscopist know if you have any allergies or you have reacted to any drugs or tests in the past
• Breathing difficulties or heart irregularities, as a result of reaction to sedation or inhaling secretions such as saliva. To help prevent this from happening, your respiration and oxygen levels will be monitored, and a suction device will be used to clear any secretions. Rarely, a heart attack or stroke (loss of brain function resulting from an interruption of the blood supply to the brain) can happen if you have serious medical problems
• Perforation – making a hole in the oesophagus, stomach (risk: 1 in 300). If a hole occurs, you will need to be admitted to hospital for further treatment which may include surgery
• Damage to teeth and bridgework. The nurse will place a plastic mouthpiece in your mouth to help protect your teeth. Let the endoscopist and nurse know if you have any loose teeth
• Bleeding from the treated are or from minor damaged caused by the dilatation. This usually stops on its own
• Incomplete procedure. This can happen due to a technical difficulty, food or blockage in the upper digestive system, complications during the procedure, or discomfort. Your doctor may recommend another endoscopy or a different test such as barium meal
• Sedation. This can occasionally cause problems with breathing, heart rate and blood pressure. If these problems do occur, they are usually short lived.
Careful monitoring by the endoscopy team ensures that any potential problems can be identified and treated quickly. Older patients and those with significant health problems such as breathing difficulties due to a bad chest may be assessed by a doctor or specialist nurse before having the procedure. If you have any further questions, please ask.
You should discuss these possible complications with your doctor if there is anything you do not understand.
References for the information contained within this leaflet if required may be obtained by the author.
People are unique and the alternatives, risks and benefits will of course vary from person to person. We hope this leaflet will support the information you have already received from your doctor in enabling you to make an informed decision about your care. If you have any questions, please ask us.
