Gastroscopy with Banding of Oesophageal Varices or Injection of Sclerotherapy
Please note, this page is printable by selecting the normal print options on your computer.
Diagram of the endoscopy procedure
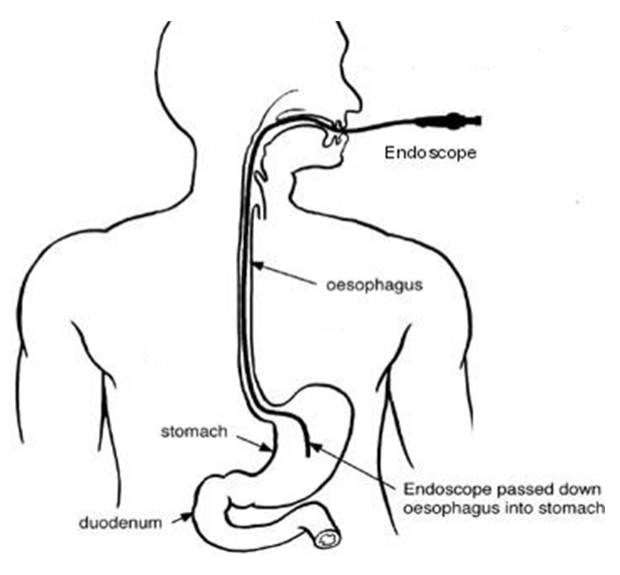
Introduction
You have been advised to have a procedure known as Banding of Oesophageal Varices or Injection Sclerotherapy. This procedure requires your formal consent. This booklet has been written to enable you to make an informed decision in relation to agreeing to the investigation. You will be required to sign a consent form on the day of the procedure, which is a legal document, therefore please read this booklet carefully beforehand. If you are unable to keep your appointment, please notify the endoscopy unit as soon as possible. This will enable staff to give your appointment to someone else and to re-arrange another date and time for you.
You need to understand all the information, including the possibility of complications. There will be the opportunity to speak to a health care professional about anything that you do not understand on the day of the procedure before you sign the consent form.
What Is an Endoscopic Treatment of Oesophageal Varices?
Oesophageal varices are dilated (enlarged) veins in the oesophagus (gullet), which if left untreated run the risk of bleeding, as the larger they become the greater the risk of heavy bleeding. Banding is a procedure that is performed, by passing a flexible telescope down into your gullet with a device attached to the tip of the telescope. This device contains several rubber bands that can be used to capture the protruding veins and “strangle” them thus reducing the risk of bleeding. It may take more than one treatment over a few months to ensure that the risk of bleeding is reduced.
Sclerotherapy is sometimes needed for treatment of varices. It involves passing a gastroscope (flexible endoscope) down into your gullet to look at the varices. A long thin tube is then passed
down the gastroscope, which has the ability to inject a sclerotherapy agent. This agent will cause the large veins to thrombose (become hard) and will reduce the risk of them bleeding. It may take
more than one treatment to ensure that the risk of bleeding has been greatly reduced by destroying the dilated veins.
How do I prepare?
To get a clear view of the oesophagus and stomach it is important that the stomach is empty. Please do not eat or drink anything for at least 6 hours before the procedure.
What about my medication?
Routine Medication
If you are on any medication, especially blood pressure tablets, you should take these with a small amount of water as usual.
Diabetes
If you have diabetes and control this with insulin or tablets, please ensure that the Endoscopy Unit is aware so that your procedure can be booked for the beginning of the list. Please see full
guidelines printed at the back of this booklet.
Anticoagulants/ Antiplatelets
If you are taking blood- thinning medicines, such as Warfarin, Dabigatran, Heparin, Dalteparin, Apixaban Clopidogrel, the dose of these may need to be altered or stopped before your procedure.
You may also need to have blood tests before your procedure. If the referring doctor did not give you instructions, you may be referred to the bridging clinic for advice on stopping your medication.
If this is required, this will be arranged for you by the referring clinician or the endoscopy booking coordinator.
What to bring with you?
Along with your appointment letter you will have received a health questionnaire. Please complete it and bring it with you. You will also find enclosed a copy of your consent form; please do not sign this until the day but read it carefully beforehand. The endoscopist or nurse will discuss the procedure, what is going to happen, any risks and any serious or common side effects. You will be given the opportunity to ask any questions before you sign the consent form. This will be done before you are taken to the procedure room.
How long will I be in the Endoscopy unit?
You should expect to be in the unit for approximately 5 hours. Please note that the time of your appointment is not the time that the procedure will be performed. How long you will be in the
unit will depend on how quickly you recover from the procedure, the sedation you may have had and also on how busy the unit is. The unit also looks after emergencies and these can sometimes take priority over outpatient procedures. You should be kept informed of any delays, but if you have any questions or concerns, please ask a member of the staff.
What happens when I arrive?
After checking in at reception, a qualified nurse will welcome you and take you to the admissions area where you will have a brief medical assessment. Please note that the endoscopy unit operates a same sex environment and your relative may not be able to accompany you past the waiting area unless there are exceptional circumstances. In the admission room, you will be asked some questions regarding your medical and surgical history to confirm that you are fit to undergo the procedure and about your arrangements for getting home. The nurse will make sure that you understand the procedure and discuss any questions you may have.
Your blood pressure, heart rate, respiration and oxygen levels will be recorded. If you have diabetes, your blood sugar level will also be checked and recorded. If you wear spectacles or dentures you will be asked to remove them when you enter the procedure room. All your belongings will be kept with you during your procedure to prevent anything being lost. You are advised to leave your valuables at home as we do not accept responsibility for them. Some people decide to have this procedure with a local anaesthetic throat spray to make the throat numb. However, some need a little bit more help to keep them relaxed.
If you have decided that you want sedation, which will be given later, the nurse will insert a cannula (a small plastic tube) into a vein in your hand or arm. All your belongings will be kept with you throughout your procedure to prevent anything being lost. It is advisable to leave any valuables at home as we do not accept responsibility for them.
Intravenous sedation
You can choose to have a sedative (usually Midazolam) which will be administered through the cannula into your vein. It will make you lightly drowsy and relaxed, but not unconscious. This means that you will still hear what is said to you and therefore, will be able to carry out simple instructions during the procedure. Some people do not remember anything about the procedure once the effects have worn off. Whilst you are sedated, we will monitor your breathing, respiration, and pulse rate via a finger probe, so that any changes can be recorded and dealt with accordingly. You will also be given some oxygen via a nasal sponge into your nostril. Your blood pressure may also be checked and recorded.
If you are having sedation, you must arrange for a responsible friend or relative to collect you and stay with you overnight. You should not drive, return to work, operate machinery, or drink alcohol for 24 hours after the procedure, nor should you make any important decisions. The reason for this is that the sedation may, despite the fact that you may feel perfectly normal, still be in the body and may impair your judgement.
The procedure
After signing your consent form in the admission area, you will be escorted to the procedure room, you will be introduced to the team and a verbal safety checklist (called “WHO”) will be done.
Your throat will be made numb by using the local anaesthetic spray; you will then be asked to lie on your left side. A “probe” will be placed on your finger which can read your pulse and the amount
of oxygen in your body (pulse oximeter). Oxygen will be given, usually via a sponge which is placed into one of your nostrils. A mouth guard is placed lightly between your teeth. During the test, photographs may be taken if appropriate. The procedure should take about 15 minutes.
Milton Keynes University Hospital is a teaching hospital and there may be a student and/or a trainee present in the room or a supervised trainee may be doing your procedure. If you have any
concerns or objections, please contact the Endoscopy Unit prior to your test or make the nurse admitting you aware of this.
Aftercare
After the procedure, you will remain in the Endoscopy Unit for between 2 – 4 hours for observation. You may feel some abdominal bloating due to the air which will have been pumped into your
stomach during the procedure.
When can I eat and drink again?
You will need to remain nil by mouth (no drink or food) for 1 hour after your procedure. You will be given written advice on what you can eat and drink when you are discharged.
When will I know the results?
Usually, the doctor or nurse will be able to tell you the results straight after the test, or if you have been sedated, when you are discharged. However, if a sample (biopsy) has been taken for
examination, the results may take several weeks. Details of results and any necessary treatment should be discussed with your general practitioner (GP) or the consultant who referred you to have
the test. A nurse will discharge you, discuss any aftercare and follow up needed and answer any questions you may have. Before leaving you should receive written information on your procedure and a copy of the consent form.
Being collected after the procedure
If you are having sedation, the person collecting you must come to the unit to collect you. We advise that they park in the multi-storey car park before reporting to the Unit.
Are there any risks?
Banding and sclerotherapy do have some risks associated with it. These occur infrequently, but we wish to draw your attention to them in order to help you make your decision. The doctor or specialist nurse who has requested the test will have considered this already. The risks must be compared with the benefit of having the procedure carried out. Complications can happen. Some of these can be serious and can even cause death (risk: 1 in 25,000). The possible complications are listed below. Any numbers which relate to risk are from studies of patients who have had this procedure. Your doctor will tell you if the risk of complications is higher or lower for you.
• Sore throat, which gets better quickly.
• Allergic reaction to equipment, materials, or sedative. The endoscopy team is trained to detect and treat any reaction that may happen. Let the admitting nurse and endoscopist know if you have any allergies or you have reacted to any drugs or tests in the past.
• Breathing difficulties or heart irregularities, as a result of reaction to sedation or inhaling secretions such as saliva. To help prevent this from happening, your respiration and oxygen levels will be monitored and a suction device will be used to clear any secretions. Rarely, a heart attack or stroke (loss of brain function resulting from an interruption of the blood supply to the brain) can happen if you have serious medical problems.
• Aspirating fluid in airway (minor risk)
• Perforation – making a hole in the oesophagus, stomach, or duodenum (risk: between 2% and 5%). The risk is higher if there are any abnormal narrowing (stricture) which is stretched (dilated). If a hole occurs, you will need to be admitted to hospital for further treatment which may include surgery.
• Damage to teeth and bridgework. The nurse will place a plastic mouthpiece in your mouth to help protect your teeth. Let the endoscopist and nurse know if you have any loose teeth or dentures.
• Bleeding from biopsy site or from minor damage caused by the endoscope. This usually stops on its own.
• Incomplete procedure. This can happen due to a technical difficulty, food or blockage in the upper digestive system, complications during the procedure, or discomfort.
• Sedation. This can occasionally cause problems with breathing, heart rate and blood pressure. If these problems do occur, they are usually short lived. Careful monitoring by the
endoscopy team ensures that any potential problems can be identified and treated quickly. Older patients and those with significant health problems, such as breathing difficulties due
to a bad chest, may be assessed by a doctor or specialist nurse before having the procedure.
You should discuss these possible complications with your doctor if there is anything you do not understand.
What to do if you feel unwell once at home?
If you ever have any signs of bleeding such as dark stools and vomiting blood, you must inform your GP immediately. If any of the above symptoms persist or worsen after your procedure – such as bleeding, pain, temperature, and shortness of breath, you must then seek urgent advice from the Endoscopy Department between 09:00 and 17:30 (01908 996460). Outside these hours, please call a nurse on Ward 8 (01908 996395) for advice or go to your nearest A&E department.
Instructions for Diabetes
You will need to adjust your treatment the evening before and the morning of your procedure to reduce the risk of hypoglycaemia (low blood sugar level). As a result, your blood sugar control may
be a little higher than usual. This is only temporary to maintain your blood sugars through the procedure and you should be back to your usual level of control within 24-28 hours after the
procedure. If you have and questions or concerns about adjusting your dosage, please contact your Diabetes Specialist Nurses well in advance of the appointment for further advice.
Carrying Glucose Monitoring
If you usually test your blood sugar levels, check them as usual on the morning of the procedure and carry your equipment with you to the appointment. If you do not usually check your blood sugar levels, please do not worry, they will be checked when you arrive for the procedure.
Tablet controlled diabetes:
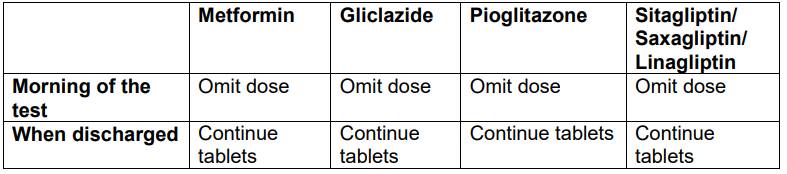
• If you are on Glibenclamide/ Chlorpropamide or Tolbutamide, change to Gliclazide by obtaining a prescription from the GP
• Test blood glucose 4-6 hourly
• Treat ‘hypos’ with a glass of Lucozade (125 ml). No Carbohydrate.
Insulin controlled diabetes:
Aim to replace your usual carbohydrate intake from the list of permitted clear fluids. You may have sugary fluids or fruit juice to replace your usual carbohydrates.
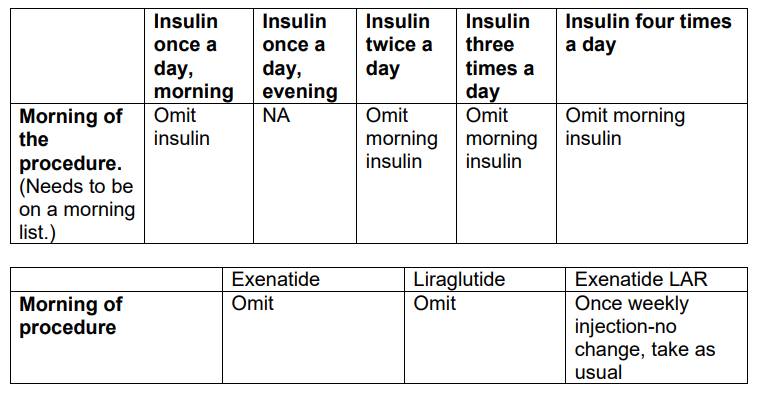
Essentials:
• 24 hours before the procedure, start testing blood glucose 2-4 hourly.
• Treat ‘hypos’ with a glass of Lucozade (125ml) no carbohydrate as on bowel prep.
• Test blood glucose before procedure.
• Bring a sandwich to eat after the procedure.
If you have concerns about adjusting your insulin dosage, please contact your Diabetes Specialist Nurse well in advance of the procedure for further advice.
References for the information contained in this leaflet may be obtained for the author.
People are unique and the alternatives, risks and benefits will of course vary from person to person. We hope this leaflet will support the information you have already received from your doctor in enabling you to make an informed decision about your care. If you have any further questions, please ask.
