Cardiac Angiography Pre-Procedure Leaflet
Please note, this page is printable by selecting the normal print options on your computer.
What is Coronary Angiogram?
A coronary angiogram is a diagnostic procedure used to detect signs of heart disease. By using X-ray with a contrast dye we can look at your coronary arteries (the vessels that supply blood to your
heart). The dye can identify if you have any narrowing or blockages by seeing how well the blood flows through the arteries (blood vessels).
The Heart
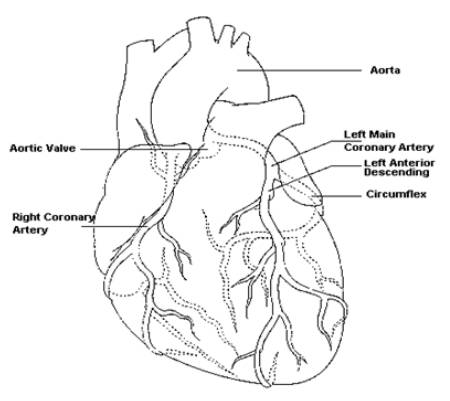
The heart is divided into four chambers called the right and left atrium and the right and left ventricle. The right side of the heart pumps blood to the lungs to obtain oxygen, the blood then
travels to the left side of the heart to be pumped around the body. The heart has its own blood supply vessels called the coronary arteries. These are the left and right coronary arteries. Heart pain, called angina, occurs when the blood supply to the heart is not sufficient enough to provide enough oxygen for the heart muscle. This pain can occur both at rest and after exertion.
Why have I been referred?
You have been referred for this procedure after careful consideration, by the health care professional (doctor or specialist nurse) looking after you based on their assessment of your symptoms at that time. Coronary angiogram not only looks at your coronary arteries to asses for Coronary Heart Disease but is also useful for investigating other conditions such as congenital heart disease.
Pre-Procedure
Please read this information book carefully, if you have any questions please bring these with you to your pre-clerking appointment or call us if no pre-assessment appointment has been given.
• If you take Warfarin, Apixaban, Rivaroxaban, Edoxaban or Dabigatran please contact the ward on 01908 996539 and ask to speak to one of the nurses, ensure you do this at least a week before your appointment.
• If you are a diabetic and take Metformin (sometimes known as Glucophage) you must NOT take it the morning of your Procedure, nor for 2 days after your procedure.
• If you are a diabetic on Insulin, please take ½ your normal dose in the morning and bring your insulin with you.
• Please bring all the medications you are taking or a list of them to the hospital with you on the day
• Your admission letter will give you details of where you need to come on the day of your procedure.
• You may wish to postpone taking any ‘water tablets’ (diuretics) on the day of the procedure and take them after your procedure has been performed.
• Please do not have anything to eat after 4.00 am on the day of your procedure. You may, however, continue to drink water ONLY prior to your procedure.
The morning of the test
We advise that you leave all valuables at home.
• You should take all your normal medications except Warfarin, Warfarin, Apixaban, Rivaroxaban, Edoxaban or Dabigatran Metformin and water tablets.
• Bring a dressing gown, comfortable footwear, book or newspaper.
On arrival, please report to the Cardiology department at the rear of the hospital site where you will be able to park in the car park B.
• It is important that you arrive on time in the morning.
• Angiograms are performed between 08.30 and approximately 16.00 hrs. Every effort is made to ensure your waiting time is kept to a minimum.
• Occasionally delays can occur; the nursing team will keep you informed of any changes.
• The Day Ward in the Cardiac suite is a single sex unit.
• Your relatives or friends will not be permitted to accompany you onto the Angiography unit however they must be available at any time on the day to come and collect you and will be
telephoned approximately 1 hour prior to your discharge. Please inform the person coming to pick you up that they should report to the main Cardiology reception desk, and the receptionist will inform us that they have arrived to collect you.
• In some circumstances it may be necessary for a relative or friend to remain in the department, in which case this will be discussed at your pre-assessment appointment, Or prior to the admission day.
The Procedure
The nurse will walk you through to the ward and ask you to get changed into a gown, they will then check your blood pressure, pulse and blood sugar if indicated. The nurse will also go through a
check list with you. A small tube called a cannula will be inserted into a vein in your arm, through this we can give you something to relax if needed and any medications required during your stay.
The doctor will then come around and go through your consent form with you and answer any questions you might have about the procedure. The procedure is carried out in a specially designed room which is set up like an operating theatre.
There will be a number of staff present throughout the procedure including:
Doctors
Nurses
Cardiac Physiologists
Radiographers
There may be staff present undergoing training.
You will be asked to walk from the Day Ward area into the Lab area; if you are unable to walk we will provide a trolley or wheelchair. The procedure normally takes about 40 minutes to perform; however it could take longer. You will be awake throughout the procedure and you will need to be able to lie flat, medication may be given to help you relax. Once inside the room you will be asked to lie on the x-ray table. A local anaesthetic will be injected into your right wrist or groin where the doctor will make a small incision. Using x-ray guidance a long narrow tube called a catheter will be passed into the artery in your wrist or groin and guided to the arteries in your heart. A contrast (liquid that shows up under x-ray) is then injected into the catheter so the arteries can be seen on the x-ray screen.
An x-ray machine will rotate around the table and take pictures as the contrast flows through your heart arteries. These pictures will be reviewed by your consultant. You will be monitored closely during and after the procedure, if you are having any discomfort please inform your nurse or doctor.
After the procedure
When the catheter is removed from your wrist or groin pressure will be applied to prevent any bleeding or bruising. If the catheter was inserted in the wrist a pressure device will be placed on the wrist after the procedure, the nurse will then gradually reduce the pressure over a period of time and the device will be removed. If the catheter was inserted into the groin a small device to stop the bleeding may be placed, allowing you to sit up straight away, if this is not done pressure will be applied to the groin to stop any bleeding. The nurse will let you know of any discharge instructions relevant to the groin before you go home.
When you return to the day ward your blood pressure, pulse and puncture site will be checked by a nurse. You may need to rest in bed until your nurse tells you it is ok to get up. The puncture site
may bleed a little after the procedure so it is important to stay in bed if your nurse tells you. You will be offered food and drink post procedure please ensure you drink plenty of water after the
procedure to eliminate the contrast from your system. Please let the nurse know if you have any specific dietary requirements when you check in.
Going home
You must: –
• Have someone to collect you from the ward at any time, as you cannot drive home or for 48 hours after the procedure. Please make sure someone is available to pick you up when we call.
• We do not advise using public transport; however if you have someone to travel with you this may be permitted.
• Have someone to stay with you overnight for the first night after the procedure, just in case the wound bleeds or you begin to feel unwell.
• Have 2 days off work following an angiogram.
• Avoid physical activity for the first few days while the puncture wound in your wrist or groin heals over completely. You can then build up activity gradually while avoiding heavy lifting. You should be back to normal activity levels within a week.
If you have any questions or problems when you have returned home you may contact the Day Ward for advice, but if you feel you need urgent assistance please contact your own GP or your
local Accident and Emergency department.
Results of the Angiogram
Your consultant or nurse will discuss the results of your angiogram and a plan of treatment with you after the procedure. If you have any questions, please do not hesitate to ask either your consultant or one of the nursing team.
Risks and Complications
Coronary angiography is generally considered to be a safe procedure. However, as with all medical procedures, there are some associated risks. This leaflet explains some of the most common side effects that some people may experience. However, it is not comprehensive. If you experience other side effects and want to ask about anything related to your treatment, please speak to the nurse at pre assessment or the consultant on the day when you sign your consent form.
The main risks of coronary angiography include:
• Bruising – it’s common to have a bruise in your arm or groin this is not serious. It is usual to expect a little tenderness for a few days following the procedure.
• Bleeding under the skin at the wound site (haematoma) – this should improve after a few days.
• False Aneurysm – This is a pulsating clot next to the hole in the artery. It will need treatment either in the form of surgery or the injection of a substance to seal the hole in the artery.
*Both haematoma and false aneurysm occur in less than 2% of procedures.
Infection
The occurrence of infection is very rare at a rate of 1 per 1000 procedures performed.
Contrast reaction
This is like an allergic reaction. If you have had problems in the past with a contrast dye you must inform the nursing staff and radiographer.
Risk of radiation from x-rays
X-rays are used as sparingly as possible and the benefits of the procedure far outweigh the risks to your health from the x-rays.
Serious complications
In very rare cases, more serious complications of coronary angiography can occur. The risk of a serious complication occurring is estimated to be less than 1 in 1,000.
These include:
• Damage to the artery in the arm or groin in which the catheter was inserted, with the blood supply to the limb possibly being affected
• Heart attack – a serious medical emergency where the heart’s blood supply is suddenly blocked
• Stroke – a serious medical condition that occurs when the blood supply to the brain is interrupted
• Damage to the kidneys caused by the contrast dye.
If you have any concerns, please contact us on the numbers given below or speak to your nurse at pre-assessment or on the day of procedure.
Other Contact details
Milton Keynes Hospital NHS Foundation Trust
Cardiac Angiography Unit
Department of Cardiology
Milton Keynes Hospital
Standing Way
Milton Keynes
MK6 5LD
Cardiac Angiography Unit 01908 996539 (Monday to Friday 8am-4pm)
If you have concerns outside normal working hours please contact the Coronary Care Unit on 01908 996419 and ask to speak to the nurse in charge for advice.
