Trans Urethral Resection of Prostate (TURP)
Please note, this page is printable by selecting the normal print options on your computer.
What is a Prostate Operation?
Introduction
We hope this patient information leaflet will support the information your surgeon has given you and help you to make an informed decision about having your prostate operation.
Why do I need this operation?
Your prostate gland sits at the base of your bladder. It surrounds your water pipe (urethra), so that if the prostate gland increases in size, it makes it more difficult to pass urine, this is because the water pipe (urethra) is being squeezed by the enlarged prostate gland.
Diagram
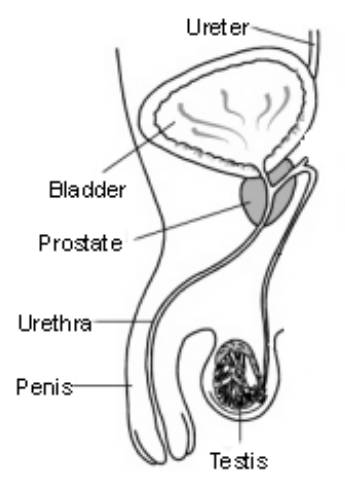
The prostate gland slowly increases in size as men grow older. Most men over fifty years old will have prostate glands that have enlarged. Usually, as men grow older, they blame their age for
‘waterworks problems’. It is partly their age, but usually it is because the prostate gland has grown.
What does the operation involve?
The operation is performed via your waterpipe (urethra) so you will not have a cut or stitches as your wound will be inside. This technique is called Trans Urethral Resection of Prostate (TURP).
The operation is carried out by a telescope and your prostate tissue is removed by a special instrument called a resectoscope (the whole of the prostate gland is not removed). This procedure allows a wider passage for urine to flow more easily. Most patients requiring this operation have it performed in this way.
What will happen if I choose not to have treatment?
If, you do not have treatment your water pipe would eventually block and you would not be able to pass urine (‘retention of urine’). If this happened you would become very poorly and need to be admitted to hospital for emergency treatment.
Pre-assessment
Usually two weeks before your operation date you will be asked to attend the hospital for a pre-operative assessment. Your appointment should take approximately one hour.
What type of anaesthetic will I have?
The type of anaesthetic you will have will be decided by your anaesthetist who will speak to you before your operation. It will usually be a general anaesthetic where you are completely asleep, or a
regional/local anaesthetic given into your back which makes you numb from the waist down.
Back on the ward….
Once you have returned back to the ward your pulse and blood pressure will be checked frequently. You will have a drip in your arm which will give you the fluid that you require until such time as you can drink normally. You will have a plastic tube (called a catheter) going into the penis. The catheter will drain the urine from the bladder while the raw area begins to heal. This may cause some discomfort at the tip of your penis.
There is always some blood loss during this operation, and this commonly continues for a while afterwards. In order to prevent the blood clotting within the bladder some fluid will flow into the catheter and out again to flush the debris and blood out satisfactorily. This flushing will continue for a variable time, but usually one or two days.
What can I do to help the operation be successful?
Lifestyle changes
• If you smoke, try to stop smoking now. There is strong evidence that stopping smoking several weeks or more before a general anaesthetic reduces your risk of complications ie. Chest infection.
• If you are overweight, you should try to lose weight.
This will also reduce your risk of developing complications.
Medications
You should continue with your normal medications. However, if you are taking Warfarin/Aspirin you will need to stop taking it before your operation. Make sure your surgeon is aware you are taking. Warfarin/Aspirin and follow advice about stopping it. Important: Before stopping any medication, you should always ask the advice of your surgeon or family doctor.
What risks or complications may occur?
Every procedure has risks and potential complications. Those most relevant to this operation are listed below:-
Complications of Anaesthetic
• When you see your Anaesthetist they will be able to discuss the risks of anaesthesia with you.
Risks and complication of this surgery……
• Pain following TURP is unusual. However, some bladder spasm or penile pain may be experienced, mainly due to the catheter.
• You may find after the operation, when the catheter is removed it is difficult to pass urine. Occasionally, the catheter may have to be put back in. If you are discharged with a catheter a District Nurse will be arranged for you.
• Bleeding is normal with this operation.
• Retrograde ejaculation. At the point of ejaculation semen would normally be expelled out through the penis. Retrograde ejaculation means that the semen goes into the bladder. This may affect your fertility but is not a reliable form of contraceptive. It does not affect your sex life.
• Impotence – the removal of the prostate tissue usually has no effect on a man’s ability to have sexual intercourse. However, a small minority between 5–10% report difficulty in getting and
maintaining erections after the operation, more so in patients who are already struggling to maintain an erection.
• Infection can occur after any operation. If, you develop a high temperature or pain on passing urine you will be given antibiotics
• Dribbling incontinence after surgery is usually only a temporary side effect, which improves in time. Therefore, if this occurs you will be advised to perform pelvic floor exercises. The exercises
will help to improve your symptoms.
• Incontinence, this may affect a small number of patients (0.2-0.3%) following TURP long-term, this may require further surgery.
• About 10% of men who have had a prostate operation will require further surgery for prostate re-growth in a ten year period.
How soon will I recover?
In Hospital
• When your urine is clear the nursing staff will remove your catheter.
• Drink plenty of water to ‘flush the system’. We recommend about two jugs of water a day as well as other drinks.
• You will be asked to use a urine collection bottle when you pass your urine, so we can monitor and measure the amount of urine you pass. It may be uncomfortable to pass urine the first few
times, but this will quickly improve. You may want to pass urine in a bit of a hurry and get little warning for the first few occasions. This will also improve fairly quickly.
Your urine output will continue to be measured throughout the day so that we can assess your progress. Once you are able to pass urine without any problems you will be allowed to go home. Most people leave hospital within a day or two of their catheter being removed.
Return to normal activities
Blood clots may be present in your urine for a number of weeks after your operation and are due to the healing process. You should drink 2-3 litres of water per day as this will help produce more urine to flush out any blood clots and help to stop urine infections. You must remember that there may be blood in your urine for at least 2–3 weeks after the operation. At first you may find that you leak some urine when straining or coughing, and that you need to go to the toilet more often. This is common and should improve over the first few weeks.
Try to drink the bulk of your daily fluids before 6.pm (this may avoid you having to get up through the night). Avoid tea, coffee, Coca-Cola, chocolate and alcohol as these may irritate your bladder.
After the operation try to eat lots of fruit and vegetables. This may prevent constipation and straining. If you strain you may find that your urine becomes slightly bloodstained.
If you become worried, or unable to pass urine do not hesitate to contact your family doctor or Urology Nurse Practitioner at the local hospital. Do not drive for the first two weeks after the
operation. Do not do strenuous exercise or lift heavy objects for six weeks after your operation as this can slow down the healing process. You may return to work in approximately 4-6 weeks after your operation depending on the nature of your job. This will be discussed with you before you are discharged home. You may resume your sexual activity 4 weeks after surgery. It is common to find blood in your semen when you begin having sexual intercourse, but this soon clears.
Will I need a follow up appointment when I am discharged?
When you leave hospital, an appointment will be made for you to see the doctor again in the outpatient clinic. This will be sent to you in the post. It is important you keep the appointment as this is a check up to make sure everything is alright and back to normal.
Further contacts:
Your GP
NHS 111
Urology Oncology Nurse Practitioner Emelda Moos: 01908 996901
Urology Nurse Practitioner Sonia Harrington: 01908 996902 Answerphone service available
