Intravitreal Injection
Please note, this page is printable by selecting the normal print options on your computer.
What is an intravitreal injection?
An intravitreal injection is an injection of a drug into the vitreous body (the jelly in the eye). It is given through the sclera (the white of the eye).
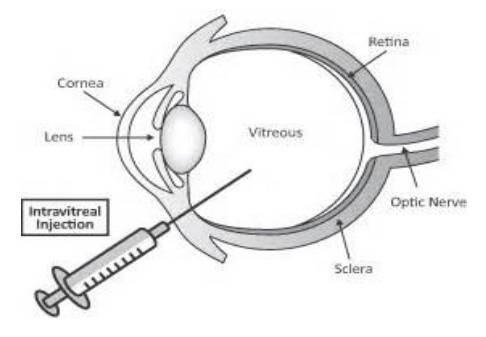
Why do I need an intravitreal injection ?
The aim of intravitreal therapy is to improve or stabilise your vision. These injections may not restore vision that has already been lost and you may experience further loss of vision caused by
the disease. The drugs most commonly used are anti-VEGF agents: Ranibizumab (Lucentis), Aflibercept (Eylea) and Bevacizumab (Avastin). In wet macular degeneration and diabetes these drugs slow or stop the growth of abnormal blood vessels in the back of the eye (retina), which are prone to leaking.
They are also used following a blocked blood vessel (retinal vein occlusion) in the eye. Anti-inflammatory drugs (steroids) such as Ozurdex are used to reduce swelling of the retina, diabetic macular oedema, retinal vein occlusion and ocular inflammation (uveitis).
Where does the procedure take place ?
Injections are performed as an outpatient procedure, either in the Eye Clinic Procedure Room or Treatment Centre. You will be given the date, time and exact location by letter or telephone call
before your treatment. These injections will be administered by a doctor or a nurse (please note there may be variation of techniques used). Expect to be in the department for approximately two
hours. The procedure takes about 20 minutes.
How do I prepare for the procedure ?
• Make sure you understand why you are having eye injections along with the potential risks of the procedure.
• Do not wear eye make-up/false eye lashes or contact lenses on the day of procedure.
• Inform the doctor/nurse if you regularly use eye medication.
• Advise of any infection or inflammation on or around the eye.
• Mention any allergies.
• Inform the doctor/nurse of any blood thinning medication e.g. Warfarin, Aspirin, Clopidrogel, Apixaban or Riveroxiban.
• Please mention to the Doctor any heart attacks or strokes in the last 3 months, or any uncontrolled high blood pressure or uncontrolled angina.
• Do not drive on the day of your appointment.
• Bring a relative, carer or friend with you. Please be aware they will not be allowed into the procedure room whilst you are having your injection.
What does the procedure involve ?
You will have local anaesthetic drops to numb the eye. The skin around your eye will be cleaned with an iodine-based antiseptic solution and some antiseptic eye drops (povidone iodine) will be
used before the injection of the drug, to reduce the risk of infection. Your face and the area around your eye will be covered by a drape (small surgical sheet) to keep the area sterile. A speculum
(clip) will be used to keep the eye open. You will be told in which direction to look and as the drug is injected it is important to keep your eye as still as you can.
Will the injection be painful ?
Although the surface of the eye will be numb from the anaesthetic drops you will probably notice a slight pressure when the needle is entering the eye, similar to that of a blood test. Any discomfort
experienced will depend on various factors as some individuals may be more sensitive than others. The speculum used to keep the eye open may cause a pressure sensation and discomfort
in some patients.
Risks of treatment and side effects?
As with any medical or surgical procedure there is a small risk of complications following intravitreal injections. For most patients the benefit of the treatment outweighs the risks.
Common side effects include:
• Pain or an ache in the eye, please take over the counter pain medication as necessary.
• Sore and gritty eye.
• Red or blood shot eye. This can look dramatic but is nothing to worry about.
• Corneal scratch.
• Floaters, shadows, bubbles, dots that may last a couple of days.
Serious but rare complications include:
• Raised eye pressure.
• Inflammation.
• Cataract.
• Retinal detachment.
• Haemorrhage (bleeding inside in the eye).
• Severe infection (endophthalmitis 1 in 2,000 cases).
• Loss of vision.
Summary
• The aim of the intravitreal therapy is to stabilise or improve your vision.
• The outcome depends largely upon your individual eye condition.
• Your eye condition may not improve or it may become worse despite these injections.
• Injections into the eye are generally safe procedures.
• Side effects may happen and some may be serious. Additional procedures may be needed to treat these complications.
• Each injection carries similar risks of developing any of the side effects or complications described.
• You must keep to the scheduled treatment and monitoring appointments so that staff can check the response to treatment and complications.
• It is not guaranteed that a particular individual will perform the procedure. The doctor/nurse will have the appropriate training and experience.
