Formation of Loop Ileostomy
Please note, this page is printable by selecting the normal print options on your computer.
Introduction
Formation of a loop ileostomy is the name given to the operation to bring out a small part of your small bowel as an ileostomy and stitch it on your tummy. The ileostomy (stoma) drains the waste from the bowel into a stoma bag. The waste from this part of the bowel is more liquid than normal bowel waste from your bottom. The operation can be done in two ways:
• It can either be performed in the traditional method of opening the tummy in a small cut where the stoma will be placed leaving a small (approximately two centimetres) wound at the side of the stoma. The wound will either be stitched or glued back together at the end of the operation and will heal in ten to fourteen days in an uncomplicated case.
• Or the operation can be performed laparoscopically. The other names for laparoscopic surgery are keyhole surgery, minimal access surgery or minimally invasive surgery.
A laparoscope is like a thin telescope with a light source. The laparoscope is passed into the abdomen through a small incision (cut) in the skin often referred to as a port. It is used to light up and magnify the structures inside the abdomen. This is then connected to a television monitor so that the surgeon can see clearly inside the abdomen.
Fine instruments are then passed into the abdomen through three or four small incisions in the skin. These instruments are used to lift, cut and take a biopsy from inside the abdomen. The decision of which method is used to perform your operation will always be made with your best interests in mind and discussed with you. However, occasionally it is necessary to abandon laparoscopic surgery if it becomes difficult to proceed safely with laparoscopic surgery.
Why do this operation?
This operation is done to divert the bowel contents away from the large bowel to allow treatment lower down in the large bowel to take place without waste matter being in the way and interfering with the treatment. The stoma nurse specialist will see you before your surgery to give you advice and support and she will give you additional written information on having an ileostomy.
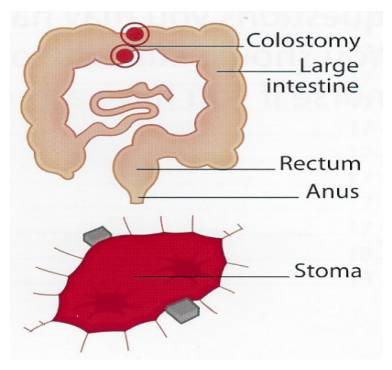
Bowel
The small bowel can be up to six metres in length. This part of the digestive tract breaks down the food you eat to allow the body to absorb all the nutrients from your food. The surgeon would bring up the small bowel onto the tummy a few centimetres from where it joins the large bowel.
Risks of this operation:
Any operation carries a risk, the risks of all operations include:
• Chest Infection. This would require antibiotics and physiotherapy.
• Blood Clots in the legs (deep vein thrombosis) or in the lung (pulmonary embolism). We decrease this risk by using elastic stockings and blood thinning injections.
• Anaesthetic. This operation is carried out under a general anaesthetic (you will be asleep). If you would like an explanation sheet about general anaesthetics and the associated risks please ask for one. If you are at increased risk because of other medical problems, you may have your consultant will refer you to an anaesthetist for a formal assessment.
• Bleeding. This can occur with any operation
• Patients who are very overweight, smoke or have other medical problems are at increased risk of all of these complications
The risks of this operation also include:
• Increased risk of infection because the bowel is an organ that is full of bacteria. This may be in the form of a wound infection. Antibiotics are given to help control the infection.
• Bowel stops working. This is temporary but can cause bloating of the tummy and sickness.
There may be more risks which are individual to you. Your consultant will discuss your individual risks with you and answer any questions you have. Measures are taken to reduce these risks; however it is not possible to stop all risks completely.
Risks of not having the surgery
Just as there are risks of having surgery there are also risks of not having surgery. These include:
• Symptoms such as pain and bleeding may become worse.
• The bowel could become completely blocked or even burst which could lead to further complications and may need surgery.
• The waste in the large bowel could also reduce the ability of the radiotherapy.
Preparation for Surgery
Your letter will inform you when to arrive at the hospital for your operation as well as when to stop eating and drinking.
After Surgery
The recovery period after bowel surgery varies. It usually involves a stay in hospital from two to seven days (in uncomplicated cases). Immediately after your operation the following tubes may be in place to help us care for you:
• Pain control may be administered through a drip (tube into the veins on your arm). This will help you move around more freely. As you recover this will be removed and pain killers will be given
in the form of tablets. The pain gradually eases, particularly once you are up and moving around
• Fluids in the form of a drip in your arm will keep you hydrated until you are able to drink freely. These tubes will be removed as soon as possible depending on your recovery. The nursing staff will help you get you out of bed as soon as possible after the operation, being mobile will help to reduce the risk of complications from the operation.
Diet
You will be able to eat during the following day but your appetite will probably be reduced. It is important to eat small frequent amounts of easily digested food. The nurse specialists can give you specific advice during this time. Meals can be supplemented with nourishing soups and snacks and high energy drinks. The body requires lots of calories during the healing process. The stoma nurse will give you detailed dietary advice.
Bowel actions
The bowel may take a little while to recover and you may still have the sensation that you need to go to the toilet in the usual way. You may even pass waste from your bottom as normal this is usually temporary but it can take some time for the large bowel to empty. Passing wind is a sign that your bowel is starting to work again. The stoma nurse will give you advice on how much output is normal and how to help reduce the amount if necessary.
Exercise
You will be encouraged to get out of bed the following day and you will be seen by a physiotherapist who will to help you do this. You will be wearing elastic stockings to reduce your risk of a blood clot but moving around will also help. The physiotherapist will also give you deep breathing exercises as this will help prevent chest infections. Lifting after abdominal surgery is not recommended for approximately four weeks after your operation. The stoma nurse will give you detailed advice on lifting.
Stoma Care
The stoma nurse specialist will see you regularly to give you help and advice on managing your stoma and you will be given all the equipment you need to do this. You have to be able to manage your stoma without help before you can be discharged home. The stoma nurse will also visit you at home within a few days after discharge to monitor your progress.
Driving
Check with your insurance company about any exclusion they may have. This includes being under the influence of some pain medication. You must be able to perform an emergency stop and you are not excluded from wearing a seat belt.
When you go home
When you go home you may find that on some days you feel better than on other days. It is quite normal to have ‘good’ and ‘not so good’ days. However it is important to contact the GP if any of the following occur:
• Discharge or leakage from the wound or drain site
• High temperature
• Uncontrolled shivering/ feeling hot then cold
• Pain when passing urine / frequent need to pass urine or very offensive smelling urine
• Difficulty with breathing, chestiness or cough with green or yellow phlegm
• Pain in the calf, leg or chest
• Abdominal pain which is different from the usual post operative soreness
• Bleeding from the back passage
• Vomiting
Confidentiality
As part of your treatment some kind of photographic record may be made. For example, photographs or video. You will always be told if this is going to happen. The photograph or video will be kept with your notes and will be held in confidence as part of your medical record. This means that it will only be seen by those involved in providing care for you or by those needing to check the quality of care you have received. The use of photographs and video is also extremely important for other NHS work, such as teaching or medical research.
If we would like to use the information for these purposes we would only do so with your permission. We do not use any information in a way that identifies you.
This information leaflet is to support and not to replace discussion between you and your specialist. Before you give your consent to any treatment you should raise any questions you have with your specialist:
Colorectal Cancer Nurse Specialist 01908 996953
Stoma Care Nurse Specialist 01908 996951
Please leave a message on our answer machine if we are not in the office.
